Pediatric Nerve Pain: How to Talk to Your Child’s Doctor
What Is Pediatric Nerve Pain?
Pediatric nerve pain, also called neuropathic pain, occurs when the nervous system sends pain signals even without ongoing injury. This type of pain feels different from a sprain or bruise and may be described as:
- Burning
- Tingling
- Electric or shooting
- Numbness with discomfort
Unlike adult neuropathy, which is often linked to diabetes, nerve pain in children more commonly develops after:
- Injury or trauma
- Viral illness
- Immune activation
- Complex Regional Pain Syndrome (CRPS)
Children’s nervous systems are still developing, which can influence how pain is processed and how recovery occurs.
Common Causes of Neuropathic Pain in Children
Pediatric nerve pain may be associated with:
- Post-viral inflammation
- CRPS
- Peripheral nerve irritation
- Autoimmune conditions
- Nutritional deficiencies
- Compression injuries
Symptoms to Describe Clearly at Your Appointment
Clear communication helps your child’s pediatric pain specialist identify patterns.
Bring a simple pain journal including:
- Intensity: 0–10 scale at rest and with activity
- Pattern: Constant or flares?
- Location: Does pain travel along a limb?
- Triggers: Movement, temperature, touch?
- Functional impact: School, sleep, sports
It can be confusing and frustrating when your child’s pain persists without clear imaging findings. Reassuring your child that their pain is real and deserves careful evaluation is an important first step.
How Is Pediatric Nerve Pain Diagnosed?
Pediatric nerve pain is often diagnosed based on a detailed medical history and neurological examination rather than imaging alone.
Your provider may recommend:
- Neurological examination
- Sensory testing
- Imaging (if trauma suspected)
- Bloodwork (to rule out underlying causes)
- Referral to specialists
In suspected cases of Complex Regional Pain Syndrome (CRPS), providers may use established clinical criteria (such as the Budapest criteria) to guide diagnosis.
In some cases, nerve conduction studies may be considered.
Treatment Options for Pediatric Neuropathy
Treatment often involves a multidisciplinary approach. Many pediatric pain programs also incorporate occupational therapy and school reintegration planning to support full functional recovery.
Physical Therapy
Supports gradual movement restoration and desensitization.
Pain Psychology
Cognitive behavioral strategies can help children cope with persistent pain.
Medications
Depending on age and diagnosis, options may include:
- Gabapentin
- Amitriptyline
- Other nerve-modulating medications
Medication decisions should always follow pediatric specialist guidance.
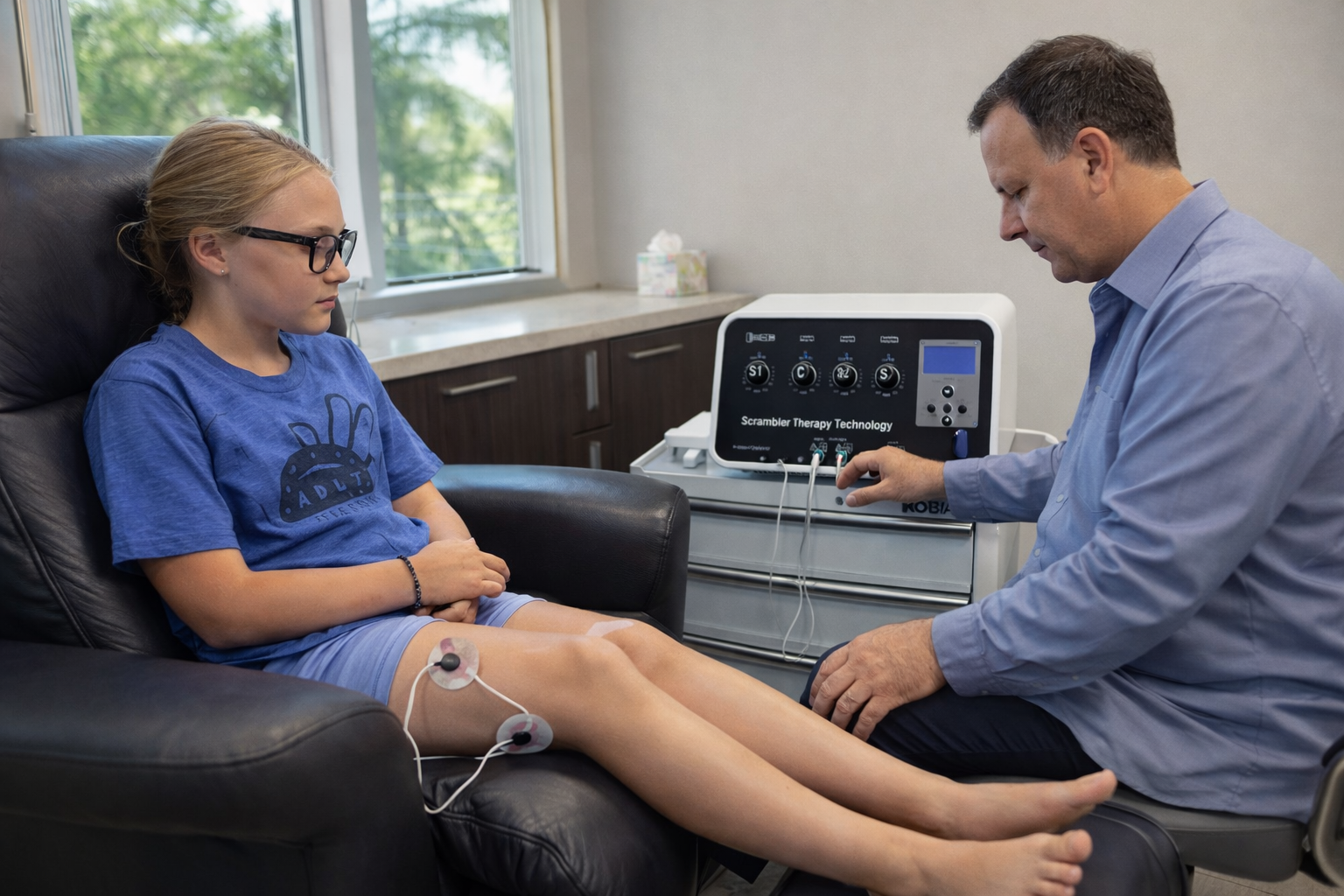
Neuromodulation Options
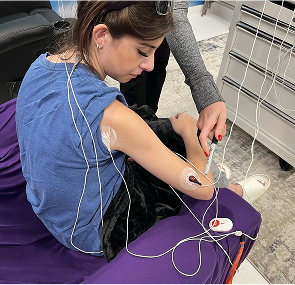
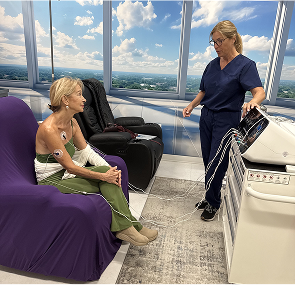
Non-invasive approaches such as Scrambler Therapy aim to modulate abnormal pain signaling. Availability varies, and not all children are candidates.
How Neuroplasticity Supports Recovery
Children have strong neuroplasticity, the nervous system’s ability to adapt.
With structured therapy:
- Pain pathways can change
- Movement confidence can improve
- Activity levels may gradually increase
Research suggests early intervention may be associated with improved functional outcomes.
When to Seek Immediate Medical Care
Seek urgent evaluation if your child experiences:
- Sudden weakness
- Loss of bladder/bowel control
- High fever with severe pain
- Rapidly worsening neurological symptoms
- Progressive numbness
Preparing for Your Appointment
Bring:
- Symptom journal
- Medication list
- Timeline of symptoms
- School impact notes
- Questions about treatment options
Frequently Asked Questions
Is pediatric nerve pain permanent?
Many children improve with structured treatment, especially when addressed early.
Is CRPS common in kids?
It is less common than adult forms but does occur and is treatable with multidisciplinary care.
If imaging is normal, is the pain real?
Yes. Neuropathic pain may not appear in standard imaging studies.
Final Thoughts
Persistent nerve pain in children deserves thoughtful evaluation. A structured, evidence-informed plan can help support gradual return to school, activity, and confidence.
If symptoms continue despite initial care, consultation with a pediatric pain specialist may help clarify next steps.
References
- International Association for the Study of Pain (IASP)
- American Academy of Pediatrics (AAP)
- Pediatric CRPS clinical guidelines
- Review articles on pediatric neuropathic pain management
Disclaimer
This article is for educational purposes only and does not replace professional medical advice.
Schedule a Pediatric Nerve Pain Consultation
If your child’s nerve pain continues despite initial care, speaking with a pediatric pain specialist may help clarify treatment options. Our team offers consultation appointments to review your child’s symptoms, prior evaluations, and possible non-surgical approaches.
👉 Schedule a Consultation or call us at +1-954-476-6661 to review your condition and explore evidence-based options.
We serve Palm Beach, Fort Lauderdale, and Miami from our location at 100 NW 100th Ave, Plantation.
You Can Follow Us through Our Social Media:
You deserve to laugh, and enjoy life without pain. The journey starts here.
Patient Reviews
Start Your Nerve Pain-Free Journey Today