When a loved one develops Complex Regional Pain Syndrome (CRPS), daily life shifts overnight. Tasks once taken for granted, buttoning a shirt, walking across a room, sleeping through the night, can suddenly become overwhelming.
For caregivers, the burden is both physical and emotional. Appointments multiply. Pain flares disrupt routines. Roles within the household change.
One caregiver described it this way:
“The hardest part wasn’t the pain itself, it was watching someone I love feel trapped inside their own body.”
Caregiver CRPS support requires more than resilience. It requires understanding the condition, protecting your mental health, and exploring structured, evidence-informed treatment pathways.
Complex Regional Pain Syndrome (CRPS) is a chronic neuropathic pain condition involving dysfunction in the peripheral and central nervous systems.¹²
CRPS is classified as:
Symptoms may include:
CRPS is often associated with central sensitization, a process in which the nervous system becomes hypersensitive and amplifies pain signaling.³
Supporting a loved one with CRPS requires organization, realistic expectations, and sustainable emotional support. A structured caregiving plan can reduce caregiver burnout and improve long-term outcomes.
Below are key tools to help caregivers navigate chronic pain more effectively.
Chronic pain caregiving can lead to emotional exhaustion and compassion fatigue. Warning signs may include:
Protecting your own mental health is essential to maintaining a stable support system.
CRPS symptoms can fluctuate unpredictably. During a flare-up:
Tracking symptom variability helps guide long-term management decisions.
Bring:
Focusing on functional restoration, not just pain scores, supports a more individualized treatment strategy.
Caregivers can support shared decision-making by asking:
Understanding risk-benefit considerations improves clarity and reduces uncertainty.
Tracking pain intensity, mobility tolerance, sleep quality, and activity triggers provides valuable data for your care team and supports structured long-term management.
While caregiver strategies provide stability at home, medical treatment remains a central component of long-term CRPS management.
CRPS is a complex neuroinflammatory and neuropathic pain condition that rarely responds to a single intervention alone.
Clinical guidelines recommend a multimodal approach, which may include:⁸
The goal is not simply pain suppression, but functional restoration and nervous system regulation.
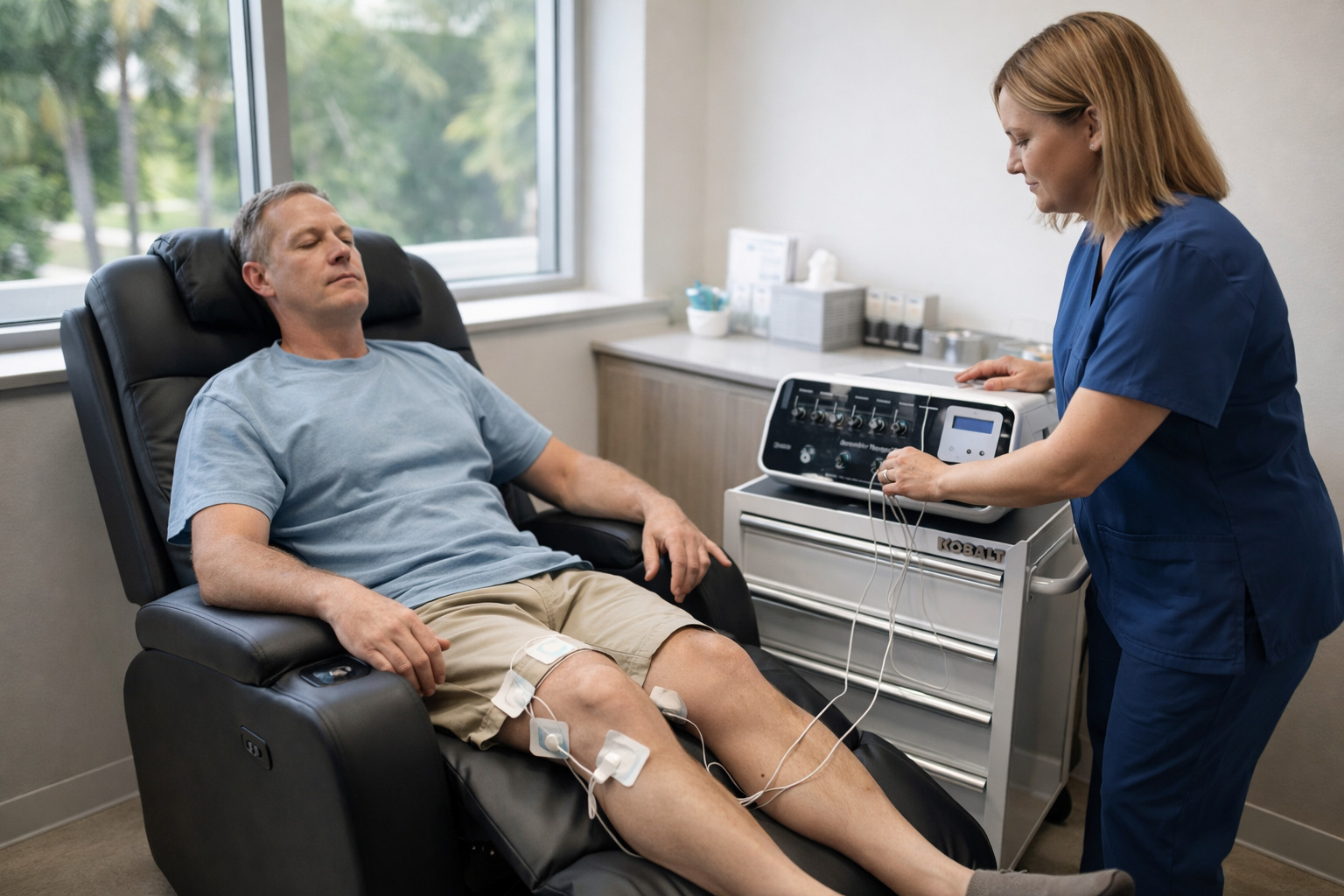
Within this framework, non-invasive neuromodulation options such as Scrambler Therapy may be considered when pain intensity limits rehabilitation progress.
Scrambler Therapy is an FDA approved therapy therapy used for neuropathic pain.
It is designed to deliver controlled electrical stimulation through surface electrodes placed near, but not directly on, the painful area.
Research suggests Scrambler Therapy may:
While the exact mechanism continues to be studied, clinical trials have demonstrated meaningful pain reduction in selected neuropathic pain populations.⁶⁷
While Scrambler Therapy has shown promising results in selected neuropathic pain populations, several important considerations should be kept in mind:
A comprehensive consultation is necessary to determine whether neuromodulation is appropriate for a specific clinical situation.
Peer-reviewed studies have examined Scrambler Therapy in neuropathic pain conditions, including CRPS and chemotherapy-induced neuropathy, showing clinically meaningful reductions in pain intensity for some patients.
However:
Balanced, evidence-informed discussions improve treatment decisions.
Pain reduction alone is not the ultimate goal.
True recovery focuses on restoring:
One patient reported that after therapy, she was able to cook independently again.
For her spouse, that milestone meant:
“I wasn’t doing everything alone anymore.”
Functional gains reduce caregiver burden significantly.
You may explore Scrambler Therapy if:
It is FDA-cleared as a medical device for neuropathic pain treatment.
Most patients describe the sensation as tingling or mild stimulation.
Durability varies. Some patients report sustained relief, while others may require repeat sessions.
No. It is often used to enhance participation in rehabilitation.
This article is for educational purposes only and does not replace individualized medical advice. Treatment decisions should be made in consultation with a qualified healthcare professional.