For many working professionals, chronic nerve pain affects more than physical comfort. It disrupts sleep, concentration, and the ability to perform consistently at work. The emotional toll, missed meetings, canceled commitments, and reduced productivity, can be as distressing as the pain itself.
For individuals experiencing post-surgical neuralgia, chemotherapy-induced peripheral neuropathy (CIPN), or diabetic neuropathy, the path back to work often feels uncertain.
“Mark,” a 42-year-old financial analyst, developed severe post-operative neuralgia after knee surgery. Although the surgical site healed, he experienced persistent electric-shock sensations radiating down his leg.
He struggled with:
“The hardest part wasn’t the pain, it was feeling like I was falling behind professionally,” he shared.
Unlike inflammatory pain, neuropathic pain is often driven by abnormal signaling within the nervous system.
After nerve injury, the spinal cord may become hypersensitive, a phenomenon known as central sensitization. The nervous system begins misinterpreting non-threatening signals as painful.
Effective treatment must address this abnormal signaling, not simply suppress symptoms.
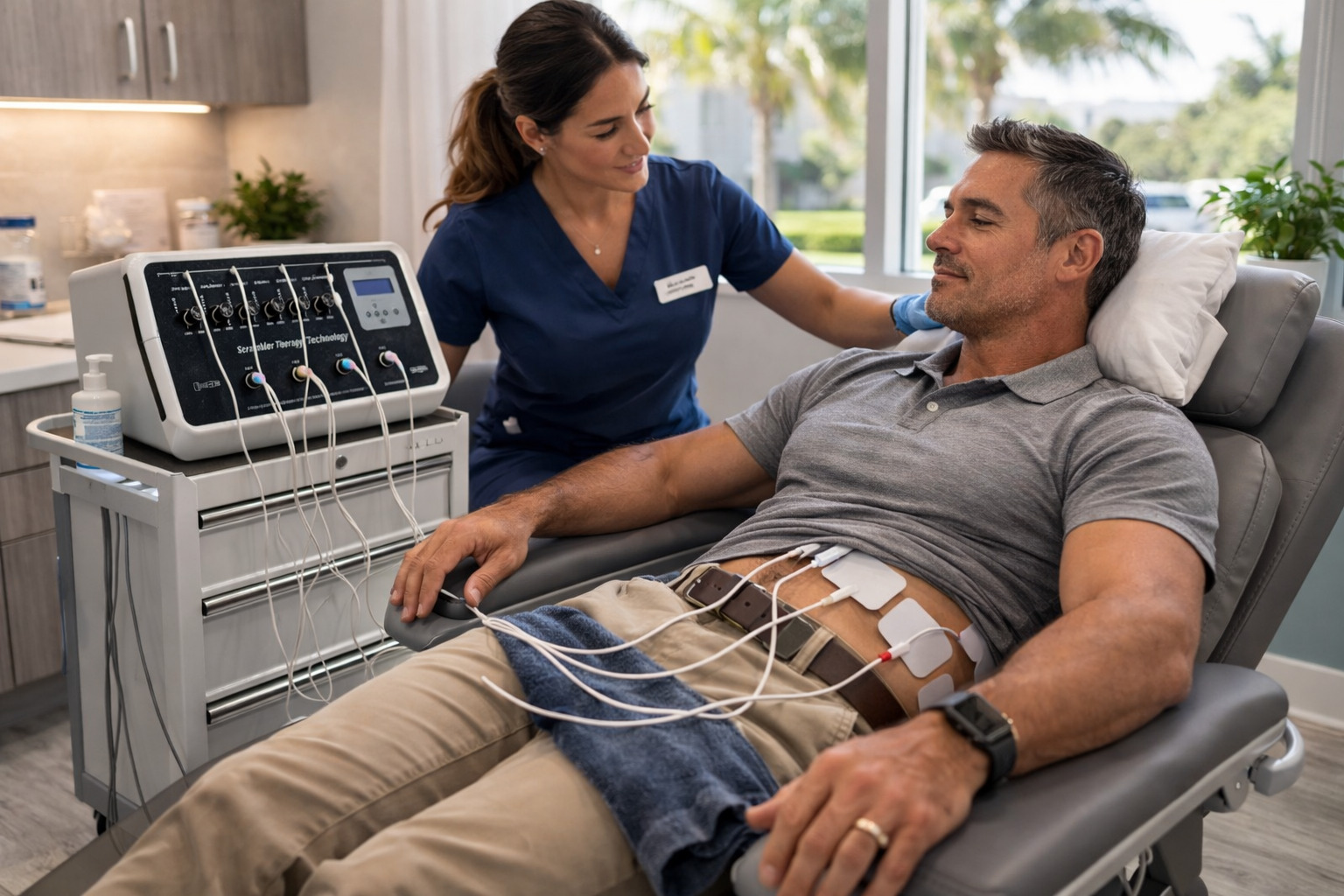
Scrambler Therapy (Calmare®) is an FDA-cleared, non-invasive neuromodulation treatment indicated for chronic pain and commonly used in neuropathic pain syndromes.
Electrodes are placed on the skin near the area of pain. The device sends synthetic “non-pain” information through the same nerve pathways that transmit pain signals, aiming to retrain how the brain interprets those signals.
It is not the same as TENS therapy. Scrambler Therapy uses a different waveform and algorithm specifically designed to modulate neuropathic pain signaling.
Although both therapies use surface electrodes, Scrambler Therapy is not a conventional TENS device. TENS delivers repetitive stimulation primarily intended to block pain temporarily. Scrambler Therapy uses variable, algorithm-driven signals designed to transmit “non-pain” information through affected nerve pathways, with the goal of retraining abnormal pain signaling over a treatment series.
Typical protocol:
Many patients report meaningful pain reduction during or shortly after the initial treatment series. However:
Before Treatment: Waking 4–5 times nightly
During Treatment Progression: Week 1 – Reduced nighttime waking; improved sleep continuity
After Initial Treatment Series: 6–7 continuous hours of sleep
Before Treatment: Unable to sit longer than 15 minutes
During Treatment Progression: Week 2 – Increased sitting tolerance; greater comfort during meetings
After Initial Treatment Series: 60+ minutes without significant discomfort
Before Treatment: Pain with short walks
During Treatment Progression: Gradual improvement during treatment
After Initial Treatment Series: 30-minute walk without cane or limping
Before Treatment: High-dose gabapentin
During Treatment Progression: Week 3 – Reduced reliance under physician supervision
After Initial Treatment Series: 50% reduction (medically supervised)
Scrambler Therapy (Calmare®) has been evaluated in multiple peer-reviewed studies investigating its role in treatment-resistant neuropathic pain, including chemotherapy-induced peripheral neuropathy (CIPN), post-herpetic neuralgia, and other chronic neuropathic syndromes. ¹–³
Notable published research includes:
As with all medical interventions, individual outcomes vary based on diagnosis, duration of symptoms, and patient-specific factors.
Scrambler Therapy is designed to address neuropathic pain driven by abnormal nerve signaling. It is not appropriate for all pain conditions.
At South Florida Scrambler Therapy, careful evaluation is performed to determine whether symptoms are neuropathic in nature. This treatment is generally not indicated for:
Scrambler Therapy does not replace necessary surgical or orthopedic care when structural abnormalities are the primary source of pain. Accurate diagnosis is essential to determine whether neuromodulation is appropriate.
Returning to work after chronic neuropathic pain often requires a structured and gradual approach. Functional recovery extends beyond pain reduction and may include adjustments that support sustained performance.
At South Florida Scrambler Therapy, patients are encouraged to consider:
Phased Return-to-Work Planning
Gradually increasing work hours or responsibilities can reduce flare-ups while rebuilding stamina.
Sitting and Standing Pacing Strategies
Alternating positions throughout the day and incorporating scheduled movement breaks may help prevent symptom exacerbation.
Pain Tracking or Journaling
Monitoring daily symptom patterns can identify triggers and guide activity adjustments during recovery.
Coordination With Employers or HR (When Appropriate)
Clear communication regarding temporary accommodations, such as ergonomic adjustments or modified duties, may support a smoother transition back to full capacity.
The goal is sustainable function. Improvement is measured not only by pain scores, but by increased tolerance for real-world activities such as sitting through meetings, commuting, and maintaining productivity.
Most patients describe the sensation as mild tingling or vibration.
Duration varies. Some patients experience prolonged relief; others may benefit from maintenance sessions.
Coverage varies and should be verified individually.
Some patients report changes within the first few sessions, though response time varies based on diagnosis and duration of symptoms.
Chronic neuropathic pain is not simply a symptom of tissue damage — it is often driven by abnormal signaling within the nervous system. When those signals become amplified or misinterpreted, daily function can decline even after the original injury has healed.
For many professionals, the goal is not just pain reduction, it is restoring the ability to work, sleep, move, and participate fully in life. When neuropathic pain is driven by dysfunctional signaling, targeted neuromodulation may offer a structured, non-invasive path toward functional recovery.
This article is for informational purposes only and does not constitute medical advice. Individual results vary.